We urgently need to pick up the pace on third doses
by Peter Breadon
Anthony Albanese campaigned on better pandemic management. Giving the vaccination program a shot in the arm will be his first test.
Not long ago, every shipment of vaccines was a news item and people were queuing around the block to get a jab.
Today, despite rising COVID cases and deaths, Australians seem to have lost interest. The vaccination rate for third doses has almost stalled.
Speeding up third doses will be critical to protecting Australians against Omicron variants as we move into winter. But without a focus on equal access, that protection will remain uneven.
Australia is losing the race
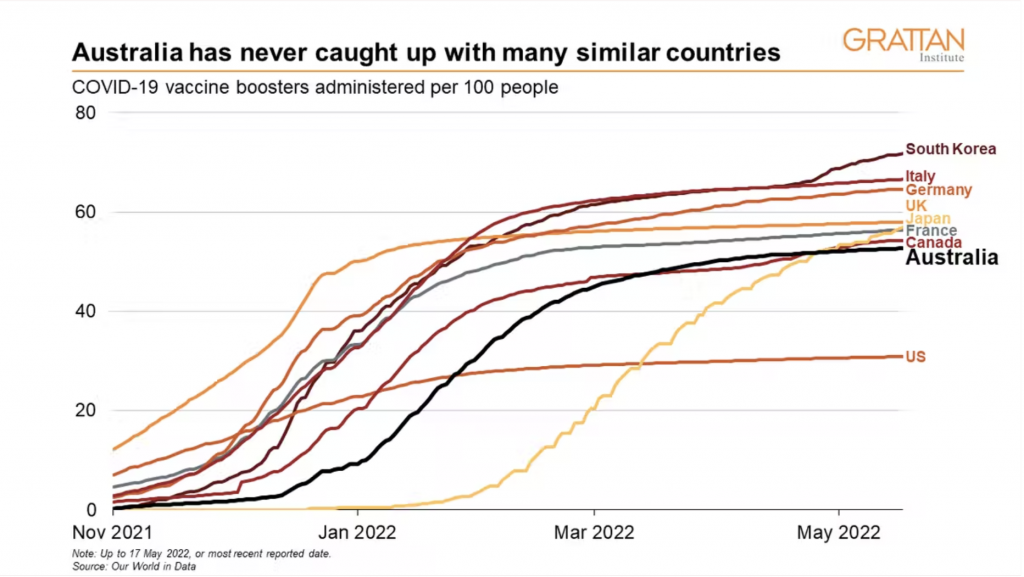
After a shaky start, Australia got near the top of the charts for second dose coverage.
But only about half the population has had a third dose. That puts us back in the middle of the OECD pack, and we’re falling further behind the leaders.

At the current rate, it would take about two years for every Australian who had a second dose to get their third. That’s not nearly fast enough to improve protection before winter.
Vaccination still matters
Thousands of hospital beds across Australia are occupied by people with COVID. Freeing up those beds is urgent.
The flu season is looming, and hospitals are facing a perfect storm heading into winter: emergency departments overflowing, elective surgery wait lists ballooning, and the health workforce stretched to the limit.
Data from the United Kingdom show third doses substantially reduce symptomatic infections and hospitalisations.
Against Omicron, protection falls quickly after the second dose, until a third dose boosts it and keeps it higher for longer.
That makes high third dose coverage important. It’s also easier than the other steps required for a comprehensive plan to cut COVID cases, such as national ventilation standards, better access to tests, more antiviral doses, and promoting mask use.
Compared to those measures, vaccination is straightforward. We’ve bought the doses, we’ve done it before, and it’s effective and safe.
But we’re moving too slowly overall, and parts of the country are being left behind.
There are wide gaps in coverage
The Department of Health publishes data on the proportion of the eligible population that has received second and third doses in different parts of Australia (the international comparison above uses the share of the whole population).
Our analysis shows that the share of eligible Australians without a third dose is three times higher in the least-vaccinated areas compared to the most-vaccinated.
This problem isn’t new. By early November in 2021, half of the local areas in Australia had reached 80% second dose coverage. Today, about one in 20 still haven’t made it.
It’s not random who misses out. Poor areas are more likely to have low vaccination rates (see chart below), even though they should have the highest.

People living in poor areas are more exposed, because more of them have in-person jobs and live in larger households. If they get infected, their chance of severe illness is higher, because they are more likely to have risk factors such as chronic disease. Low vaccination coverage only adds to their risk of harm.
Likewise, people living in remote areas have lower vaccination, as do Aboriginal people in many parts of Australia, even though these groups are at greater risk.
A key lesson of Victoria’s second wave in 2020, and NSW’s in 2021, is the importance of vaccinating people at higher risk, including those in lower-income areas, to slow the spread of COVID and reduce severe illness. The data show this critical lesson of the pandemic has not been learned.
How can we get faster … and fairer?
Getting higher – and fairer – vaccination rates will require national and local action.
Government advertising and political leadership helped raise the vaccination rate before. The Albanese government should lead the way on third doses, promoting the importance, safety, and impact of vaccination.
The government should set ambitious coverage targets for vulnerable groups and areas, and support tailored, local solutions to achieve them.
Primary Health Networks (PHNs) are regional bodies responsible for improving primary care, which is health care given outside a hospital, typically without a referral. That includes vaccinations at GP clinics and community pharmacies. Their role includes improving access to care for people at risk of missing out. PHNs should work with local communities to lift third dose rates, with new funding for the PHNs that have the lowest rates in their area, linked to targets they must hit.
Local barriers are different from place to place, but there are many proven ways to overcome them. Clinics reaching out to people is effective. Aboriginal-controlled services can play a critical role in their communities. There is experience here and overseas about partnering with community leaders and organisations, countering distrust, and vaccinating in different community settings.
Tough vaccine mandates have worked to increase uptake. If other measures fail, and hospitalisations rise, they should be considered again.
Without strong leadership, the vaccination rate will remain low and uneven. Getting it right will make a difference now and give us the playbook for the next dose, the next vaccine, and the next pandemic.
Peter Breadon
While you’re here…
Grattan Institute is an independent not-for-profit think tank. We don’t take money from political parties or vested interests. Yet we believe in free access to information. All our research is available online, so that more people can benefit from our work.
Which is why we rely on donations from readers like you, so that we can continue our nation-changing research without fear or favour. Your support enables Grattan to improve the lives of all Australians.
Donate now.
Danielle Wood – CEO
