Race to 80: how we mapped Australia’s path out of the COVID crisis
by Stephen Duckett, Will Mackey
Earlier this month National Cabinet released a four-phase COVID response plan. It wasn’t so much a plan – it had no dates and no thresholds – but more a back-of-the-napkin thought bubble. It was sensible, but vague.
National Cabinet now faces the hard task of converting vagueness into a real plan. To do this it must answer the question: what proportion of the Australian population needs to be vaccinated before we can open our international borders?
This means allowing stranded Australians to return, letting footloose people travel overseas, and welcoming international tourists and students again.
Well qualified experts differ on the requisite threshold for vaccination partly because there are so many unknowns, such as how quickly the Delta variant of COVID would spread through Australia if we open up, and how effective the different vaccines will prove to be in preventing transmission.
But new Grattan Institute modelling shows it would be dangerous for Australia to open up before at least 80% of the population is vaccinated.
Here’s what we found, and how we came to the 80% figure. Let’s start with the good news.
Vaccines offer substantial protection
Both vaccines on offer in Australia – Pfizer and AstraZeneca – are effective at preventing infections from the Delta strain. Two doses of Pfizer offers about 88% protection against infection, while two doses of AstraZeneca offers about 67% protection.
Vaccinated people can still catch COVID, but those that do pass it on to about half as many others compared to the unvaccinated.
Evidence from the United Kingdom, Canada, and the European Union – areas with higher vaccination levels than Australia – also suggests both vaccines offer substantial protection against hospitalisation and death from COVID. A vaccinated person is about 95% less likely than a vaccinated person to end up in hospital with COVID.
Now for the bad news.
The delta strain is far more infectious
Researchers estimate the Delta variant is 50% to 100% more infectious than the Alpha variant, which itself was more transmissible than the variant that was dominant throughout 2020.
The effective reproduction number, or Reff, tells us how many people one infected person will spread the virus to, taking into account behaviour and public health measures in place designed to reduce transmission, such as masks and physical distancing.
If the Reff of the Delta variant in Australia is around 6 without vaccination, having 50% vaccination coverage will reduce the Reff to 3.
But the national goal must be to bring the Reff down to below 1, which would mean each person who was infected would infect less than one other person – and the virus would eventually peter out.
The higher the vaccination rate, the lower the effective reproduction number. Each person vaccinated offers a chance of breaking a chain of transmission that might lead to an outbreak.
Not only are vaccinated people less likely to become infected, they are also less likely to pass the virus onto others if they are.
The higher the vaccination rate, the lower the effective reproduction number
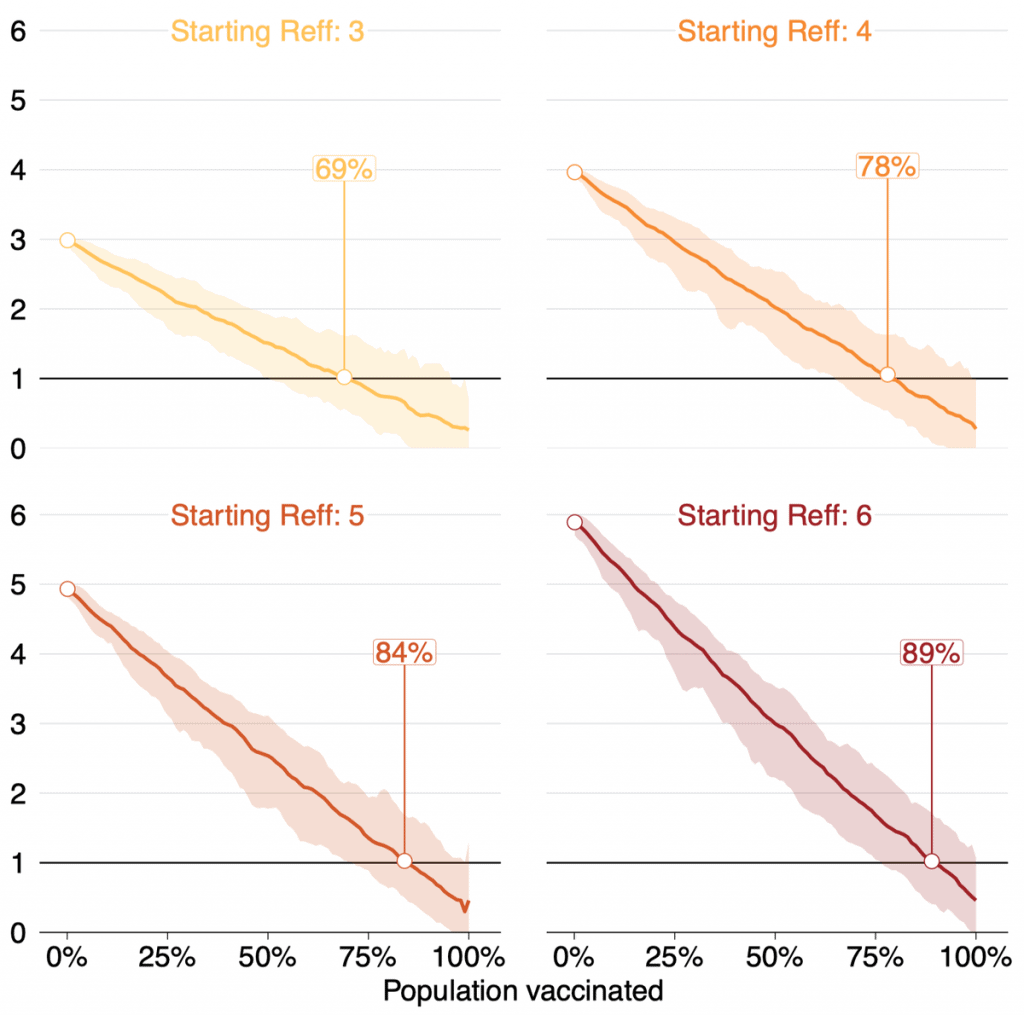
So why do we need 80% of people vaccinated?
Grattan Institute’s model simulates the spread of COVID within a partially vaccinated population, and helps us peek into the future.
It uses age-based hospitalisation and intensive care unit (ICU) admission rates from more than a year of COVID data from Australian ICU units. It also assumes children under 16 are about one-fifth less likely to get COVID, and children over the age of two are able to be vaccinated.
In most of our simulations, older people have higher rates of vaccination, and no age group has more than 95% vaccine coverage.
We ran thousands of simulations of different vaccination rates, and different estimates of the Reff. The outcomes for 12 distinct scenarios are shown in the table below.
You can see why we recommend Australia not open up until at least 80% of the population is vaccinated – it is the only scenario where the virus is managed, with hospitalisations and deaths kept down to reasonable levels, even if the Reff is high.
What are the risks of opening up at different levels of vaccination?
Modelling for COVID-19 outbreak at different levels of vaccination, by virus Reff value.

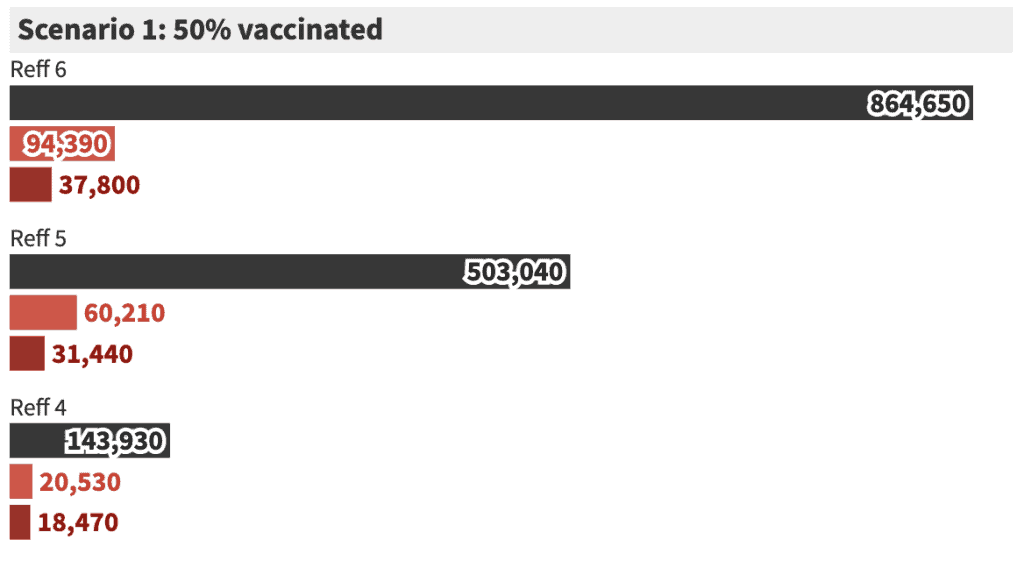

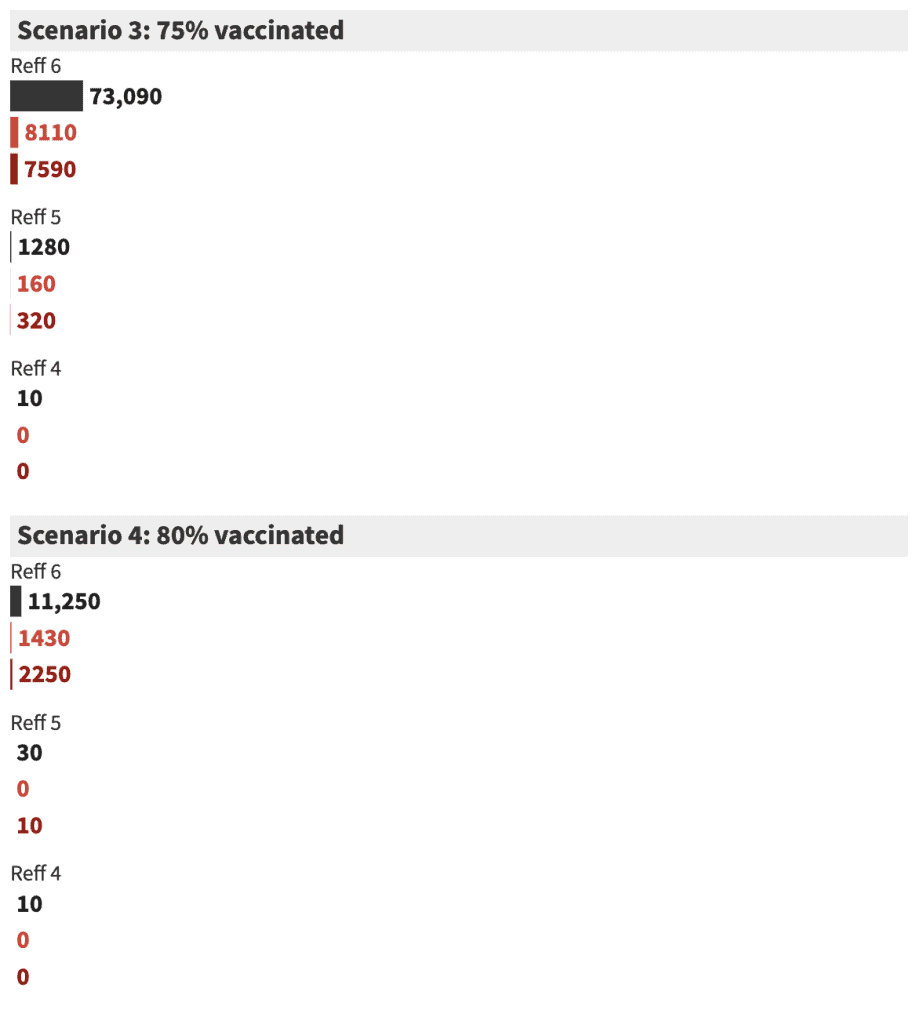
Let’s break it down
Our simulations show that opening up at 50% vaccination rate (scenario 1) is a very bad idea, with many, many thousands of deaths.
Scenarios 2 and 3 are the optimist’s and gambler’s scenarios. If you are lucky and the Reff of Delta in Australia is 4 (with 70% vaccination rate) or 5 (with 75% vaccination rate), deaths and hospitalisations would not rise above moderate levels, and lockdowns could end and the borders could reopen.
But if you gambled on the wrong Reff, our hospitals would be overwhelmed and deaths would be unacceptably high. Opening the borders is a one-shot gamble: if you make the wrong call, the virus will quickly spread and all the good work and hard yards of living through lock-downs over the previous two years will have been wasted.
Public health decision-making is often risk averse, for the best of reasons. The difference in virus spread, hospitalisations and deaths between opening at 75% and at 80% are big, but the wait between the two thresholds may only be a month or two. This is why we recommend an 80% vaccination rate (scenario 4) as the threshold for opening up.
Even if the Reff of Delta is 6, our hospital system will not be overwhelmed, and deaths will not rise above the number of deaths in a moderate flu season, such as 2010, when there were 2,364 flu deaths.

Will Mackey
While you’re here…
Grattan Institute is an independent not-for-profit think tank. We don’t take money from political parties or vested interests. Yet we believe in free access to information. All our research is available online, so that more people can benefit from our work.
Which is why we rely on donations from readers like you, so that we can continue our nation-changing research without fear or favour. Your support enables Grattan to improve the lives of all Australians.
Donate now.
Danielle Wood – CEO
